3D Mammography
3D Mammography
By Adam Braithwaite, M.D.
I am a son, husband and father of three daughters. As you can imagine, women’s health is a priority for me and I have dedicated my life to the pursuit of detecting breast cancer early so that it can be treated and cured.
For years, screening mammography has been our primary tool in this fight. In fact, since regular screening mammography began in the United States in the 1980s, breast cancer deaths have plummeted 35 percent. That is fantastic, but there are limitations in women with dense breasts, which have more fibrous or glandular tissue in relation to fatty tissue.
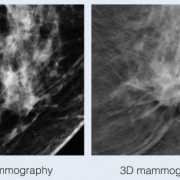
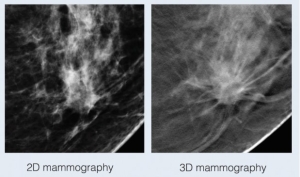
With traditional mammograms, it can be difficult to detect cancers in dense breasts because the images are acquired in two dimensions and the breast is a three-dimensional structure.
This can lead to overlapping tissue, which can obscure a small mass or mimic an invasive cancer. Usually these overlapping areas can be cleared with additional images and ultrasound but “false positive” call-backs cause a great deal of anxiety for women. This is where breast tomosynthesis, also known as 3D mammography, can help.
This breakthrough in breast imaging utilizes advanced imaging technology to produce a three-dimensional image of the breast with multiple slices through the tissue, similar to a CT scan.
Consider the difference between a chest x-ray and CT scan. When we look at the x-ray image, the heart, lung, skin, and bones all overlap and small lung nodules can hide. With a chest CT, we can look at these structures from the inside – slice by slice – and detect even the smallest cancer.
3D mammography separates tissues and reduces overlapping of structures, resulting in improved cancer detection and reduced callback rates for benign findings. A study in the American Journal of Radiology showed that tomosynthesis has improved detection of invasive aggressive breast cancers, up to 41 percent, and a 29 percent increase in the detection of all breast cancers.
There was also a 15 percent decrease in the number of women called back from screening exams. That means less anxiety and stress each year for a large number of women and fewer unnecessary tests and biopsies for those areas that cannot be cleared by standard mammograms and ultrasound.
There is a slight increase in radiation with 3D mammography but the FDA has deemed it safe for use as an annual screening tool. In addition, minimal increase in radiation will likely be offset by the decreased additional imaging needed for those false positive callbacks.
3D mammography also gives greater detailed information on the initial screening exam that will allow many women to proceed directly to ultrasound and be spared additional x-rays for diagnosis, further decreasing radiation exposure.
On a personal note, 3D mammography saved the life of my mother. Her doctors were able to find a small invasive cancer that would not have been seen with 2D mammograms. As a result, the cancer was still small and had not spread to her lymph nodes. She was treated with surgery and radiation therapy and is now cancer free.
Please discuss with your doctor if breast tomosynthesis would be a good option for you.

Adam Braithwaite MD, is a Duke Fellowship Trained Breast Imager, formally trained with the interpretation of tomosynthesis. Dr. Braithwaite is a member of the team at Delaney Radiologists, 1025 Medical Center Drive, Wilmington, NC.